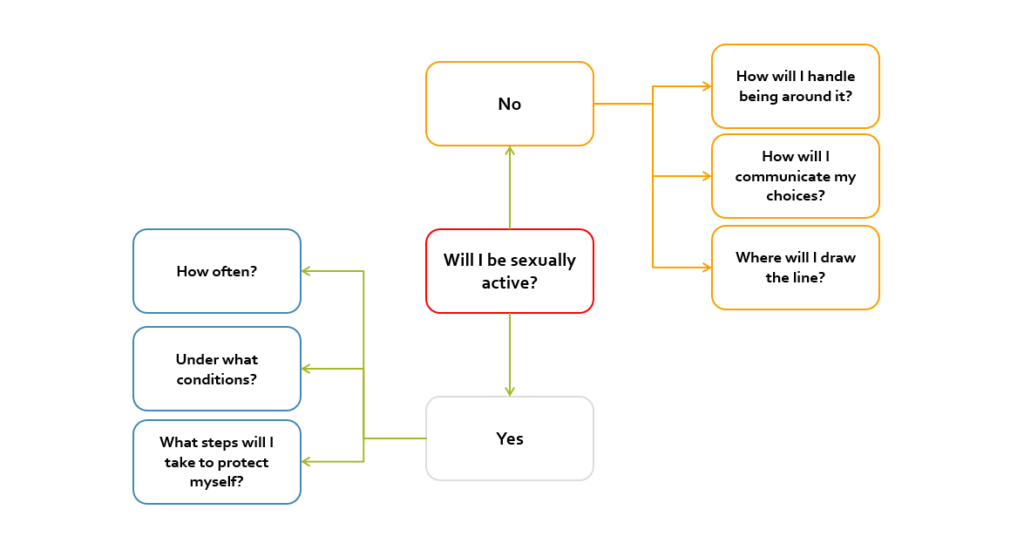
College is a time of choices regarding sexual activity. How and when to make choices such as whether to remain celibate or to become or remain sexually active are important facets of the college experience.
Interest in interpersonal sexuality naturally ebbs and flows. Sex affects our emotional state, no matter how experienced we are sexually, from encounters that leave us feeling exuberant, contented, or excited, to those that leave us confused, scared, depressed, or angry. Mentally categorizing an encounter as a hookup or casual does not mean we won’t have to deal with feelings about it.
Jump to resources and educational websites.
The bottom line is that we need to be aware of our sexual feelings and treat them with respect, doing only what we feel is right.
As you make your sexual health decisions, remember that the best decisions are informed decisions.
Check out the campus, community, and online resources provided on this website.
Make your sexual health a priority.
You have a right and a responsibility to be active in your decision making.
It’s your decision—think it through.
Birth Control
By openly discussing birth control prior to a sexual relationship, partners do more than prevent pregnancies. Such sharing enhances mutual trust and caring, and increases the likelihood of using the chosen birth control successfully. Some feel that raising the topic of birth control in an intimate situation interferes with spontaneity and romance—this is a myth that needs to be dispelled. It is when birth control is not discussed that spontaneity goes out the window and mutual respect is undermined. Romance is better preserved, in both causal and long-term relationships, when birth control is acknowledged as a shared responsibility.
Which Method to Choose
Choosing a birth control method, like choosing a sexual partner, depends mostly on individual preferences. What’s right for one person may not work for another. More importantly, what works may not be appropriate later on as lifestyles and relationships change. Therefore, birth control methods need to be reevaluated from time to time.
Deciding which method to use can be a confusing process. Make an appointment with the Women’s Clinic at the Student Health Center or ask a medical professional of your choice.
Many people get their sexual information or expectations from the media. Countless figures in the entertainment industry serve as powerful role models, but rarely do these images of sexuality and sexual health accurately reflect true sexual realities.
To first get an idea of what options are available, Bedsider.org provides information on all of the different birth control methods and even includes a comparison tool.
STIs
Sexually Transmitted Infections (STIs, sometimes referred to as STDs) are infections or diseases that are passed from one person to another during sexual contact (oral, vaginal, and anal sex). STIs include chlamydia, gonorrhea, herpes, HIV, HPV, and syphilis. Some STIs, such as herpes and HPV, are transmitted via skin-to-skin contact. STIs are common among young adults aged 24 and younger, with 15-24 year olds making up half of all new STIs in the United States.
Preventing STIs
You can reduce the risk of STIs by using barriers correctly, every time during sexual activity. Barriers include male condoms (external condoms), female condoms (internal condoms), and dental dam.
These barriers can be obtained for free from the Safer Sex and Safety Wall located at the Center for Health Education & Wellness office located on the second floor of the Student Health Building, Monday – Friday 8:00am – 5:00pm.
Learn how to use a male condom (external condom) correctly:
Learn how to use a female condom (internal condom) correctly:
Treating STIs
Sexually active individuals should get tested at least once a year. Many STIs do not have symptoms, or have symptoms that are similar to other health issues. Many young adults will have an STI and not realize it. For example, 1 in 7 people living with HIV do not know that they are positive.
The only way to know whether or not you have an STI is to get tested. The Student Health Center provides STI testing.
Even though some STIs cannot be cured, all STIs can be treated. It is important to get tested and get treatment for STIs to avoid more serious health issues. Only a healthcare provider can test for STIs and prescribe any necessary treatment.
COVID-19 and Sexual Health
COVID-19 is not considered an STI. At this time, sexual transmission is not known to have caused a case of COVID-19, but because COVID-19 is primarily spread through close contact with respiratory droplets physical intimacy poses a risk.
The National Coalition of STD Directors and NASTAD (a non-profit association of public health officials) have created a FAQ that can help you better understand the risk of COVID-19 and how to reduce those risks: Sex and COVID-19: Frequently Asked Questions.
Information adapted from:
American Sexual Health Association Creating a Healthy Nation
CDC.gov
Women’s Health.gov
Campus Resources
- Need Condoms?
- Pride Center
- Student Counseling Center
- Student Health Center
- Student Health Center’s Women’s Health Clinic